
Loud snoring is often ignored until it starts affecting daily life. When it is paired with daytime fatigue, it may indicate sleep apnea, a condition where breathing repeatedly stops during sleep.
Many individuals assume they are simply not getting enough rest. In reality, the issue is often interrupted breathing cycles that prevent deep sleep.
Recent estimates suggest that over 900 million adults worldwide may have obstructive sleep apnea, with a large percentage remaining undiagnosed. Early awareness is key to preventing long-term complications.
What Is Obstructive Sleep Apnea?
Obstructive sleep apnea (OSA) occurs when the airway becomes partially or completely blocked during sleep. These blockages can happen multiple times per hour, leading to repeated pauses in breathing.
This results in:
- Reduced oxygen supply
- Frequent sleep interruptions
- Poor sleep quality despite adequate duration
Over time, this affects both physical and mental health.
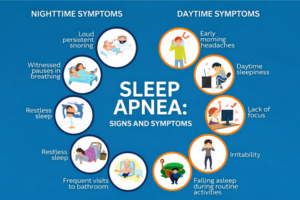
Early Signs of Sleep Apnea You Should Not Ignore
Sleep apnea often develops silently, and many individuals do not realize they have a problem until it begins to affect their daily life. Recognizing the early warning signs can help in seeking timely diagnosis and preventing long-term complications.
Loud, Persistent Snoring
Frequent and loud snoring is one of the earliest and most noticeable signs of sleep apnea. It usually occurs due to narrowing or blockage of the airway during sleep. If snoring is consistent and disruptive to others, it should not be ignored.
Excessive Daytime Fatigue
Waking up feeling unrefreshed despite adequate sleep is a common symptom. Interrupted breathing prevents the body from reaching deep, restorative sleep stages, leading to constant tiredness, low energy, and daytime drowsiness.
Gasping or Choking During Sleep
Sudden awakenings with a choking or gasping sensation are often linked to pauses in breathing. These episodes may go unnoticed by the individual but are frequently observed by family members.
Morning Headaches
Reduced oxygen levels during sleep can result in dull headaches upon waking. This symptom is often overlooked but can be an important indicator of disrupted breathing patterns.
Poor Concentration, Memory Issues, and Irritability
Sleep disruption directly affects brain function. Individuals may experience difficulty concentrating, forgetfulness, mood swings, and irritability, impacting both personal and professional life.
Why Sleep Apnea Is a Serious Health Concern
Sleep apnea is more than just a sleep disturbance—it is a medical condition that can significantly affect overall health. Repeated interruptions in breathing reduce oxygen supply and place stress on the body over time.
If left untreated, sleep apnea can increase the risk of:
- High blood pressure
- Cardiovascular disease
- Type 2 diabetes
- Stroke
- Reduced productivity and overall quality of life
Early diagnosis and appropriate treatment can greatly improve sleep quality, energy levels, and long-term health outcomes.
Why Sleep Apnea Is a Serious Health Concern
Sleep apnea is not just a disturbance of sleep—it is a medically significant condition that can affect multiple systems in the body. Repeated interruptions in breathing lead to reduced oxygen levels and increased strain on the heart and brain.
If left untreated, sleep apnea can significantly increase the risk of:
- High blood pressure (hypertension)
- Cardiovascular disease, including heart attacks
- Type 2 diabetes
- Stroke
- Reduced productivity, daytime performance, and overall quality of life
Clinical evidence shows that untreated moderate to severe sleep apnea is strongly associated with an increased risk of cardiovascular complications. Early diagnosis and appropriate management are essential to prevent these long-term health consequences.
Causes and Risk Factors of Sleep Apnea
Sleep apnea can develop due to a combination of anatomical and lifestyle-related factors that affect airway stability during sleep.
Structural Factors
Certain physical characteristics can narrow or block the airway, especially during sleep:
- Naturally narrow airway
- Enlarged tonsils or adenoids
- Deviated nasal septum affecting airflow
Lifestyle Factors
Daily habits and health conditions can increase the likelihood of airway collapse:
- Excess body weight, particularly around the neck
- Alcohol consumption before sleep, which relaxes airway muscles
- Smoking, which contributes to airway inflammation
Emerging Trends in Sleep Apnea
Recent clinical observations show that sleep apnea is no longer limited to older or overweight individuals. It is increasingly being diagnosed in a broader population.
Growing trends include:
- Rising cases among younger adults
- Increased prevalence in individuals with sedentary lifestyles
- Higher risk in people with irregular sleep schedules and excessive screen exposure
This shift highlights the importance of early awareness, timely evaluation, and lifestyle modification to prevent progression and complications.
How Sleep Apnea Is Diagnosed
Diagnosing sleep apnea requires a comprehensive evaluation that combines clinical assessment with specialized sleep testing. Early and accurate diagnosis is essential for effective treatment planning.
Clinical Evaluation
An ENT specialist performs a detailed examination to identify any structural causes that may be contributing to airway obstruction. This includes:
- Assessment of the nose, throat, and airway
- Identification of conditions such as a deviated septum or enlarged tonsils
- Evaluation of breathing patterns and medical history
Sleep Study (Polysomnography)
A sleep study is the gold standard for confirming sleep apnea. It monitors:
- Breathing patterns
- Oxygen levels in the blood
- Heart rate and sleep stages
This test helps determine the severity of the condition and guides the choice of treatment.
Airway Assessment
Advanced airway evaluation may be recommended to understand the exact site and degree of obstruction, allowing for a more targeted treatment approach.
Treatment Options for Sleep Apnea
Treatment for sleep apnea is not one-size-fits-all and is carefully tailored based on the severity of the condition, underlying anatomical factors, and overall health of the patient. A detailed evaluation helps determine whether the condition is mild, moderate, or severe, and identifies the exact cause of airway obstruction.
Depending on these findings, management may include a combination of non-surgical therapies and ENT-based interventions aimed at improving airflow, stabilizing breathing during sleep, and preventing long-term complications.
Non-Surgical Management
- CPAP (Continuous Positive Airway Pressure) therapy to keep the airway open during sleep
- Weight management to reduce airway narrowing
- Positional therapy (avoiding sleeping on the back)
- Avoiding alcohol and sedatives before bedtime
ENT-Based Treatment
- Correction of nasal obstruction (e.g., deviated septum)
- Tonsil or soft palate procedures to widen the airway
- Minimally invasive airway surgeries for selected cases
A personalized treatment plan ensures better outcomes and long-term symptom control.
When to See an ENT Specialist
You should seek medical evaluation if you experience any of the following symptoms regularly:
- Loud snoring on most nights
- Persistent daytime fatigue or sleepiness
- Observed pauses in breathing during sleep
- Morning headaches
- Difficulty concentrating or memory issues
Early consultation can help prevent complications and significantly improve quality of life.
Common Myths About Sleep Apnea
Many misconceptions about sleep apnea prevent individuals from recognizing the seriousness of the condition and seeking timely treatment. Misunderstanding these myths can delay diagnosis and increase the risk of long-term health complications. Understanding the facts is essential for making informed decisions about your health.
- “Snoring is harmless” → Persistent snoring can be an early warning sign of sleep apnea
- “Only overweight individuals are affected” → Structural airway issues can cause sleep apnea even in individuals with normal weight
- “Sleep apnea is rare” → It is a common but widely underdiagnosed condition
Key Takeaways
- Loud snoring and daytime fatigue are early indicators of sleep apnea
- The condition disrupts breathing and reduces oxygen levels
- Untreated sleep apnea increases the risk of serious health problems
- Diagnosis through a sleep study is essential
Early treatment improves sleep quality and overall health
Frequently Asked Questions
1. Is loud snoring always a sign of sleep apnea?
No, loud snoring is not always a sign of sleep apnea. However, persistent loud snoring combined with daytime fatigue, choking episodes, or breathing pauses during sleep significantly increases the likelihood of obstructive sleep apnea. If these symptoms are present, medical evaluation is recommended.
2. Can sleep apnea be treated without surgery?
Yes, sleep apnea can often be treated without surgery, especially in mild to moderate cases. Common non-surgical treatments include CPAP (Continuous Positive Airway Pressure) therapy, lifestyle modifications such as weight management, positional therapy, and avoiding alcohol before sleep. Treatment depends on the severity and underlying cause.
3. How dangerous is untreated sleep apnea?
Untreated sleep apnea is a serious health condition that can lead to long-term complications. It is associated with an increased risk of high blood pressure, heart disease, stroke, type 2 diabetes, and reduced cognitive function. Early diagnosis and treatment are essential to prevent these risks.
4. What is the best sleeping position for sleep apnea?
Sleeping on your side is considered the best position for sleep apnea, as it helps keep the airway open and reduces obstruction. Sleeping on the back (supine position) can worsen symptoms by allowing the tongue and soft tissues to collapse backward.
5. Can young or fit individuals have sleep apnea?
Yes, sleep apnea can affect individuals of all ages and body types. Even young or physically fit individuals may develop sleep apnea due to structural airway issues such as a narrow airway, enlarged tonsils, or a deviated nasal septum.
6. How is sleep apnea confirmed?
Sleep apnea is confirmed through a sleep study (polysomnography), which monitors breathing patterns, oxygen levels, and sleep stages. An evaluation by an ENT specialist helps identify structural causes and determine the most effective treatment plan.
Dr. Sudarshen Aahire is a young, talented, and vibrant ENT and Pediatric doctor in Nashik with 12 years of experience. Apart from routine ENT care and surgeries he specializes in the management of Snoring and obstructive sleep apnea surgeries, Endoscopic skull base surgeries, voice-related disorders, and voice surgeries, airway and swallowing disorders.

